Breathing is something most of us take for granted until it suddenly becomes difficult. If you’ve noticed persistent shortness of breath, unexplained tiredness, or chest discomfort, it can be alarming. One possible cause that often goes undiagnosed in the early stages is pulmonary hypertension.
Pulmonary hypertension is a serious but manageable medical condition. With better awareness, early diagnosis, and modern treatment options, many people are now living longer and healthier lives. This guide will help you understand pulmonary hypertension clearly—without complicated medical jargon—so you can make informed decisions about your health.
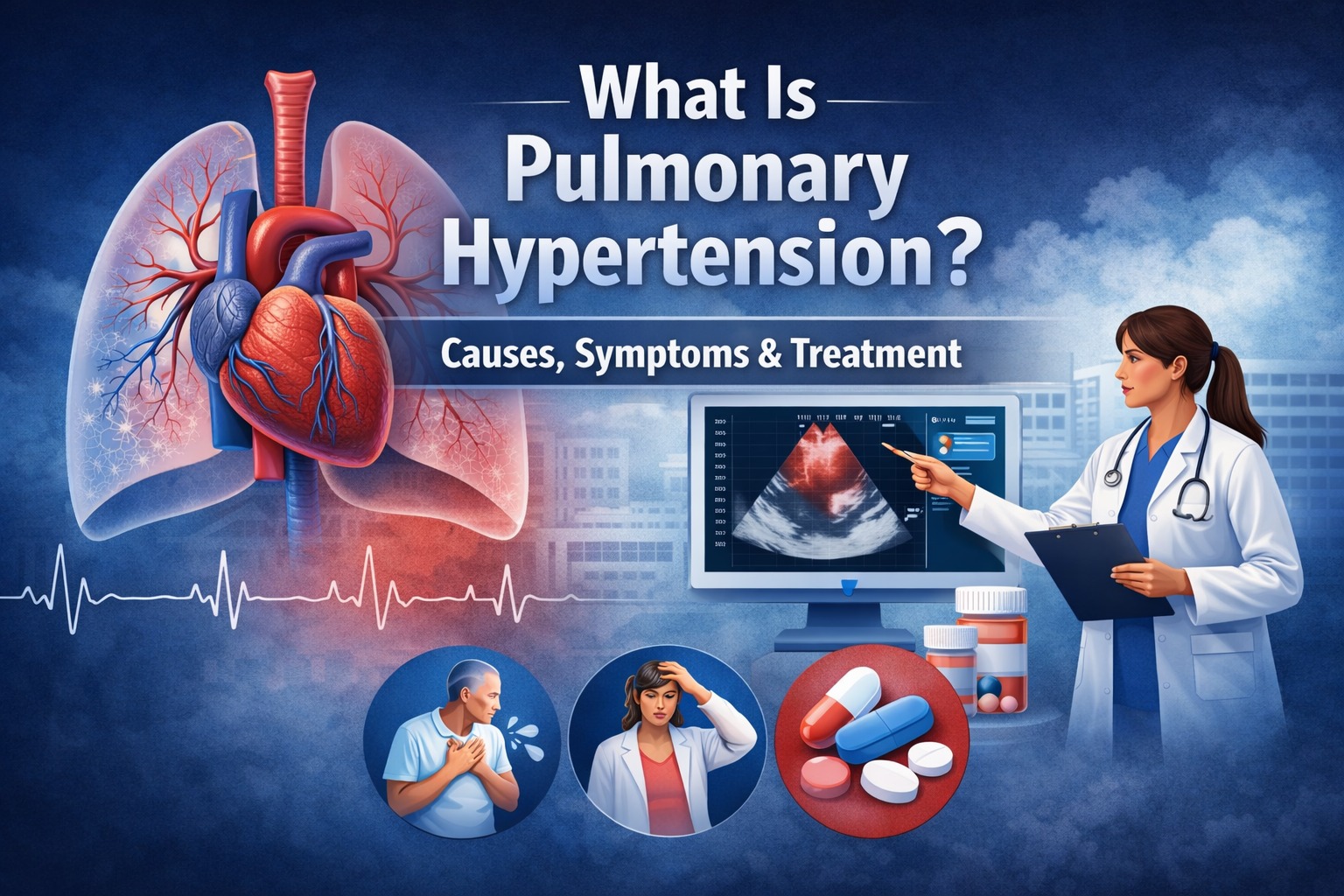
What Is Pulmonary Hypertension?
Pulmonary hypertension (PH) is a condition in which the pressure in the pulmonary arteries blood vessels that carry blood from the heart to the lungs becomes abnormally high.
Under normal conditions, blood flows easily through the lungs to pick up oxygen. In pulmonary hypertension, the pulmonary arteries become narrowed, stiff, blocked, or damaged, making it harder for blood to pass through. As a result, the heart, especially the right side—must pump harder to move blood forward.
Over time, this extra workload can weaken the heart and lead to right-sided heart failure if not treated.
👉 Important to remember: Pulmonary hypertension is not the same as regular high blood pressure measured in the arm. A person can have normal blood pressure readings and still suffer from pulmonary hypertension.
What Is Pulmonary Arterial Hypertension (PAH)?
Pulmonary Arterial Hypertension (PAH) is one of the more serious forms of pulmonary hypertension. In PAH, the small arteries within the lungs undergo structural changes, including:
- Thickening of artery walls
- Narrowing of blood vessels
- Reduced blood flow to the lungs
This leads to decreased oxygen delivery throughout the body and increased pressure on the heart. PAH is considered a progressive condition, but modern treatments have significantly improved outcomes.
With timely diagnosis and specialist-guided care such as that provided at Pulse Multispecialty Hospital many patients experience better symptom control and improved quality of life.
Types of Pulmonary Hypertension
Pulmonary hypertension is not a single disease. Instead, it is an umbrella term used to describe five different groups of conditions, each with its own causes, treatment approach, and long-term outlook. Understanding the type of pulmonary hypertension you have is extremely important, because treatment that works for one type may not be suitable for another.
Doctors classify pulmonary hypertension based on how and why the pressure in the lung arteries becomes elevated.
Group 1: Pulmonary Arterial Hypertension (PAH)
Pulmonary Arterial Hypertension (PAH) is one of the most serious and well-known forms of pulmonary hypertension. In this condition, the small arteries inside the lungs become narrowed, thickened, or stiff, making it difficult for blood to flow through them.
As resistance increases, the heart must pump harder to push blood into the lungs, leading to increased strain on the right side of the heart.
PAH may occur due to:
- Unknown causes (idiopathic PAH)
- Genetic or inherited conditions
- Autoimmune diseases such as scleroderma or lupus
- Certain heart defects present from birth
- Long-term use of specific medications or drugs
PAH is usually progressive, but with early diagnosis and modern targeted therapies, symptoms can be controlled and disease progression can be slowed significantly.
Group 2: Pulmonary Hypertension Due to Left Heart Disease
This is the most common type of pulmonary hypertension and is often seen in people with long-standing heart problems.
In this group, pulmonary hypertension develops because the left side of the heart cannot pump blood efficiently. As blood backs up, pressure increases in the lungs.
Common causes include:
- Left-sided heart failure
- Mitral or aortic valve disease
- Cardiomyopathy (weakened heart muscle)
- Long-standing high blood pressure affecting the heart
Treatment focuses on managing the underlying heart condition, rather than targeting the pulmonary arteries directly. When heart function improves, lung pressure may also decrease.
Group 3: Pulmonary Hypertension Due to Lung Diseases or Low Oxygen Levels
Group 3 pulmonary hypertension occurs when chronic lung disease or low oxygen levels damage the pulmonary arteries over time.
This type is commonly linked to:
- Chronic Obstructive Pulmonary Disease (COPD)
- Interstitial lung disease
- Sleep apnea
- Pulmonary fibrosis
- Long-term exposure to high altitudes
Low oxygen levels cause the lung arteries to tighten, increasing pressure. Management focuses on treating the lung condition and improving oxygen levels, often with oxygen therapy.
Group 4: Chronic Thromboembolic Pulmonary Hypertension (CTEPH)
CTEPH is caused by old or repeated blood clots in the lungs that fail to dissolve properly. These clots block or narrow the pulmonary arteries, leading to persistent high pressure.
What makes CTEPH unique is that:
- It may develop months or years after a pulmonary embolism
- Symptoms often progress gradually
- It is potentially curable in many cases
Treatment options may include:
- Blood-thinning medications
- Surgical removal of clots (pulmonary endarterectomy)
- Balloon pulmonary angioplasty in selected patients
Early diagnosis is critical for achieving the best outcomes.
Group 5: Pulmonary Hypertension With Unclear or Multiple Causes
This group includes cases of pulmonary hypertension that do not fit neatly into the other categories or have multiple contributing factors.
Possible causes include:
- Blood disorders such as anemia or myeloproliferative diseases
- Metabolic conditions
- Inflammatory or systemic diseases
- Tumors pressing on pulmonary blood vessels
Because this group is complex, treatment is highly individualized and often involves managing the underlying condition while closely monitoring pulmonary pressure.
What Causes Pulmonary Hypertension?
Pulmonary hypertension develops when something interferes with the normal flow of blood through the lungs. Over time, this interference increases pressure in the pulmonary arteries, forcing the heart to work harder than it should. Understanding the causes is important because treatment often depends on addressing the underlying problem.
In many cases, pulmonary hypertension does not have just one cause—it can result from a combination of medical conditions and lifestyle factors.
1. Heart Diseases
Conditions affecting the left side of the heart, such as heart failure or valve disease, can cause blood to back up into the lungs. This increased pressure in the pulmonary arteries over time leads to pulmonary hypertension, especially when heart problems remain untreated or poorly controlled.
2. Chronic Lung Diseases
Long-term lung conditions like COPD, interstitial lung disease, or pulmonary fibrosis reduce oxygen levels in the blood. Low oxygen causes pulmonary arteries to tighten and narrow, increasing pressure inside these vessels and eventually leading to pulmonary hypertension.
3. Blood Clots in the Lungs
Repeated or untreated blood clots in the lungs can block pulmonary arteries. Over time, these blockages raise pressure in the lung circulation, causing chronic thromboembolic pulmonary hypertension, a serious but potentially treatable form of the disease.
4. Autoimmune and Connective Tissue Disorders
Diseases such as lupus, scleroderma, or rheumatoid arthritis can damage blood vessels throughout the body, including the lungs. This damage causes narrowing of pulmonary arteries, increasing resistance to blood flow and leading to pulmonary hypertension.
5. Genetic and Unknown Causes
In some people, pulmonary hypertension is inherited or develops without a known cause. Genetic mutations can affect how pulmonary blood vessels function, causing them to narrow or stiffen over time, even in otherwise healthy individuals.
Treatment Options for Pulmonary Hypertension
While pulmonary hypertension may not always be curable, effective treatments can control symptoms, slow disease progression, and improve daily life.
Medications
Treatment may include:
- Vasodilators to relax pulmonary arteries
- Medications that reduce blood vessel narrowing
- Drugs that improve blood flow
- Blood thinners to prevent clots
- Diuretics to reduce fluid retention
Oxygen Therapy
Oxygen therapy helps improve breathing, reduces heart strain, and enhances overall comfort for patients with low oxygen levels.
Advanced Treatments
In selected cases:
- Balloon pulmonary angioplasty
- Surgical removal of clots (for CTEPH)
- Lung or heart-lung transplantation
Lifestyle Changes That Support Recovery
Along with medical treatment, lifestyle adjustments play a key role:
- Light, doctor-approved exercise
- Low-salt, heart-healthy diet
- Avoid smoking and alcohol
- Maintain a healthy weight
- Manage stress and emotional well-being
- Stay up to date with vaccinations
These steps help reduce symptoms and support long-term health.
Prognosis and Long-Term Outlook
The outlook for pulmonary hypertension varies depending on:
- Type and severity of the condition
- How early it is diagnosed
- Response to treatment
- Overall health and lifestyle
With today’s medical advances, many people with pulmonary hypertension lead active and meaningful lives.
Living With Pulmonary Hypertension
A diagnosis of pulmonary hypertension can feel overwhelming, but you are not alone. With expert care, personalized treatment, and ongoing support, managing this condition becomes possible.
At Pulse Multispecialty Hospital, patients receive comprehensive evaluation and advanced care for heart and lung conditions under one roof. The focus is always on early diagnosis, compassionate treatment, and long-term well-being.
Conclusion
Pulmonary hypertension is a complex condition, but knowledge is the first step toward control. If you notice symptoms or have concerns, don’t ignore them. Early medical attention can make a life-changing difference.
With the right care and guidance, pulmonary hypertension can be managed—and life can move forward with confidence.